 For those of you who did not make it to the latest GIM Training Day at Newham here are some GIM pearls from the talks.
For those of you who did not make it to the latest GIM Training Day at Newham here are some GIM pearls from the talks.
Asthma – from getting the basics right to beyond step 5
Dr Nivenka Jayasekera highlighted the results of The National Review of Asthma Deaths which reported that 3 people die from asthma a day, and that 2 of these are preventable. Several issues were highlighted in both the acute and chronic management of those who died. In particular there was underuse of preventer inhalers, and over-reliance on salbutamol. Importantly those that died were in all groups on the treatment ladder (step 1 and step 5).
We were encouraged to remember the underlying pathology, and to get the basics right to save lives.
Acute management:
- Assess severity, using PEFR and ability to complete sentences. RR or wheeze can be misleading.
- Prioritise nebs and steroids early. Give magnesium if severe/life-threatening attack (often given very early), and aminophylline only if life-threatening (poor evidence).
- Continue the patient’s usual combination inhaler (often missed/stopped).
- NIV for asthma should NOT be given on the ward, only in ICU with ability to intubate rapidly if required
- Assess inhaler technique and adherence. Assess triggers.
- iv salbutamol is only appropriate if not able to get in nebs (ie on ICU in patient with high airway pressures) – it has side effects (tachycardia, lactataemia, arrhythmia) so should not be given outside ICU
- Discharge is a key time to make a difference:
- smoking cessation advice and referral
- inhaled steroids and rescue pack with self-management plan
- inhaler technique check
- PEFR metre and chart to take home as part of self-management plan
- see GP within 2 working days
- Respiratory OP appointment in 4-6 weeks
Chronic management:
- BTS guidelines provide a step by step guide
- Moving up the steps should be triggered by waking at night monthly or more often, or using salbutamol inhaler weekly or more
- Concordance is often an issue. In a study by Prof Liam Heaney in Belfast, patients on step 5 were ‘confronted’ using cortisol levels (objective evidence of regular inhaled/oral steroid use), and when presented with this evidence admitted non-adherence (45% of those prescribed oral steroids!). This is not necessarily an approach we advocate…
- Beyond step 5:
- check IgE levels and consider referral to a specialist centre for omaluzimab (which is more expensive than gold by weight! and has miraculous effects in some patients)
- Other options include methotrexate, 3 x weekly azithromycin, sc turbutaline, desensitisation, regular review or clinical trials
- investigations may include HRCT, FeNO, sputum and/or BAL for inflammatory cells, bronchial biopsy, oscillometry, and alveoscopy (research tool)
Worryingly, symptoms do not always correlate with disease severity. Airway remodelling is a key part of the pathogenesis, which is not necessarily measured by spirometry/peak flow/exacerbation rate. Phenotyping of asthma is important but not well understood. The most worrying group are those with discordant inflammation (ie on step 1 due to low symptoms, but high levels of inflammation identified in a trial by bronchial biopsy). Future research may help identify this group and treat pro-actively (although as pointed out by an audience member ensuring good concordance may be challenging).
We were wowed with some immunology – remember that there is more to life than just Th1 and Th2 – the discovery of new T-cell subsets such as the IL-17–producing TH17 and T-regulatory cells has changed our understanding of T-cell biology and chronic inflammation. This may open the door to potential future therapies.
HIV emergencies for the medical SpR
 Dr Tommy Pasvol started by testing our knowledge of the STDs of the famous. Did you know that Manet and Al Capone are both believed to have had neurosyphilis, and Billy Idol spoke to Rolling Stone magazine about his genital herpes? Of course there are also many famous people who had/have HIV. PHE produced figures for STDs based on modelling for 2012 that suggested there were 100,000 HIV infected individuals, 77% diagnosed, 73% retained in care and 58% with undetectable. The prevalence of HIV is increasing, incidence decreasing (since people are living longer). In the UK prevalence is 1.5/1000 (47/1000 in MSM and 83/1000 in London MSM). There are ethnic differences with 31/1000 Black African men and 64/1000 Black African women (easier for women to contract). Is is therefore common. It has been proved to be cost effective to test since late diagnosis has huge implications in terms of cost, morbidity and mortality.
Dr Tommy Pasvol started by testing our knowledge of the STDs of the famous. Did you know that Manet and Al Capone are both believed to have had neurosyphilis, and Billy Idol spoke to Rolling Stone magazine about his genital herpes? Of course there are also many famous people who had/have HIV. PHE produced figures for STDs based on modelling for 2012 that suggested there were 100,000 HIV infected individuals, 77% diagnosed, 73% retained in care and 58% with undetectable. The prevalence of HIV is increasing, incidence decreasing (since people are living longer). In the UK prevalence is 1.5/1000 (47/1000 in MSM and 83/1000 in London MSM). There are ethnic differences with 31/1000 Black African men and 64/1000 Black African women (easier for women to contract). Is is therefore common. It has been proved to be cost effective to test since late diagnosis has huge implications in terms of cost, morbidity and mortality.
General medical registrars are most likely to encounter new diagnoses in patients presenting with other associated conditions, or emergencies in patients who are known to be positive.
Top tips:
- don’t forget the usual medical differential, as many positive patients are on treatment and have normal CD4 counts so are at risk of the same conditions as any immunocompetent patient
- determine the level of immunocompromise quickly by getting access to recent CD4 and viral load and looking for cachexia, oral candidiasis, Kaposi’s Sarcoma, lymphadenopathy, and poor skin eg folliculitis, psoriasis, and molluscum
- document full past medical history, current and previous drugs and prophylaxis
- enquire about adherence, adverse drug events, and starting/stopping treatment
- get a travel history
- PCP (pneumocystis jiroveci) is a diagnosis made on sputum MC+S (PCR less specific). There is a normal chest x-ray in 39%. BHIVA guidelines advocate iv co-trimoxazole and prednisolone.
- “Pott’s puffy tumour” is osteomyelitis of a frontal bone abscess from inhaled drug use
- Toxoplasmosis is present in a high proportion of the general population: 10-40% of the UK, 90% French are toxo serology positive. Investigations include toxo serology, serum CrAg, blood and sputum cultures and LP. Treatment is with pyrimethamine + sulphadiazine (+folinic acid). After 2/52 secondary prophylaxis is given. Usually steroids are not indicated. ARVs should be started 2 weeks after treatment for toxo is started.
- Cryptococcal meningitis is treated with amphotericin B and flucytosine. Therapeutic LPs are required if CSF pressure >19mmHg. Maintenance treatment is with fluconazole until immunocompetent.
- JC virus leads to PML. It affects white matter only leading to demyelination. >70% of the population are serpositive. it has a very poor prognosis in HIV/AIDS.
- CMV retinitis gives the classical “pizza pie appearance” and is treated with oral valganciclovir (SE of nephrotoxicity and marrow toxicity).
- Remember syphilis – it is making a comeback! Particularly in the MSM community.
- In patients with rectal discharge test for LGV and Shigellosis
- Seroconversion is primary HIV infection and is a time of high infectivity. Patients may be HIV antibody negative (eg POC tests). Need to do bloods for p24 antigen and HIV RNA. Start ARVs if neurological involvement or AIDS defining illness.
- The SPARTAC trial in NEJM randomised patients to early ARVs or standard care. It showed that a 48-week course of ART in patients with primary HIV infection delayed disease progression, although not significantly longer than the duration of the treatment. Therefore it did not change practice.
- Drug reactions may present on the acute take. Abacavir (an NRTI in Kivexa) hypersensitivity is associated with HLA-65701 – cytotoxic T cels are produced. Patients should be tested before treatment. Other drug reactions can occur, particularly with NNRTIs. eg pancreatitis (DDI), lactic acidosis (AZT, D4T), psych disturbance (efavirenz), renal stones (Pis).
- A useful app for drug interactions and adverse effects is HIV i-chart. For opportunistic infection guidelines get the BHIVA app.
Valvular heart disease
Dr Kula Ranjadalayan reminded us of the common symptoms of valvular disease: breathlessness, chest pain, palpitations, syncope, ankle swelling, and fatigue. More uncommon symptoms include: upper GI symptoms (RH failure), jaundice (RH failure), TIA/CVA (embolic from MS), haemoptysis (MS), hoarse voice (MS due to LA enlargement – Ortner’s syndrome).
Remember the respiratory manoeuvres that will help you hear murmurs: at the left sternal edge TR is worse on inspiration and VSD is worse on expiration.
ECGs can indicate valvular disease:
- LA enlargement – mitral valve disease P mitrale
- LVH (deep S in V2, tall R in V6) – aortic valve disease, MR
- RVH – MS, PS, TR
- AF – mitral or aortic disease
- AV block – aortic valve disease
- Biatrial enlargement – MS
But what we really need are handheld ECHOs (which could also be used to ultrasound any other part of the body too of course)! If only they were a bit more affordable. I don’t have a spare £5000, sadly. If you do, please send it my way.
From an ECHO we can get multiple views. M-mode is used to take measurements. 2D images allow measurement, assessment of LV and RV function (eg parasternal and long axis view). Colour Doppler allows direction of flow assessment for regurgitant jets. Doppler velocity adds additional information.
Other cardiac investigations for valve work-up include: cardiac MRI, cardiac catheterisation of R and L heart and CT heart for TAVI planning.
Mitral stenosis is usually rheumatic or congenital. Valve area determines severity, with severe <1cm^2. LA size and RA pressure are important. Treatment is diuretics/B-blocker/digoxin for AF, consideration of warfarin, percutaneous balloon mitral valvulotomy, or mitral valve replacement. Indications for valvotomy are: symptoms with moderate/severe MS; asymptomatic but PASP >50mmHg; and if not suitable eg mixed valve disease then refer for surgery (repair or replacement).
Mitral regurgitation has a number of causes. Primary: mitral valve prolapse, flail, degeneration, rheumatic, infective endocarditis. Secondary: LV disease, IHD, dilated cardiomyopathy, hypertrophic cardiomyopathy, papillary muscle rupture (leads to acute pulm oedema). Surgery is indicated for: acute MR; chronic severe MR with symptoms; and, if asymptomatic, LVEF <60%, LVEF >60% and systolic diametes >45mm, or LA dilatation, AF, high PA pressure and raised BNP.
Aortic stenosis is caused by age-related degeneration, bicuspid aortic valve, or rheumatic disease. Severe is mean aortic valve gradient of >40mmHg. Valve area < 1cm^2 is severe. Indications for surgery include: severe symptoms; indications for a CABG with symptoms; or asymptomatic but with a positive exercise test, or raised BNP. If not suitable for surgery TAVI is an option.
In aortic regurgitation LV size and function is important. Surgery is indicated in acute AR, chronic severe AR with symptoms, or if asymptomatic with LVEF <50%, or >50% and end-diastolic diameter >70, or end-systolic diameter <50.
Dementia – pitfalls of diagnosis in the acute setting
Dr Kris Warren discussed the National Dementia Strategy from the Department of Health 2009. It states that early intervention enhances quality of life, delays or prevents admission to a care home, and is cost effective. Patients with dementia have poor access to palliative care, and poor end of life care. They are less likely to get analgesia (as they may fail to communicate the fact that they are in pain explicitly). Many patients have multi-morbidity, with only 5% having a single diagnosis of dementia.
Dementia cannot be diagnosed in the acute setting. Confounders include: delirium; language or cultural differences; sensory impairment; and depression and anxiety. It is also easy to miss dementia in the acute setting: in mild Alzheimer’s, unless you see the patient regularly it is easy to miss mild symptoms; patients with subcortical dementia (usually vascular) will score well on simple screens, but will be slow; patients with executive dysfunction will also score well on simple screens; those with Lewy Body dementia are often diagnosed as recurrent delirium (eg said to have UTIs with minimal evidence). Another important alternative diagnosis to dementia is depression. Depression can present with physical and cognitive signs and symptoms that mimic dementia. The two conditions require entirely different treatments, so misdiagnosis cna have terrible consequences.
If undiagnosed there is an increased risk of readmission and recurrent admissions. It is likely dementia contributes to an inability to manage other co-morbidities well. There is a difference between cognitive impairment and dementia. Dementia is progressive, and affects multiple domains of functioning.
Dr Warren impressed upon us the fact that dementia is a specialist diagnosis. However, identifying patients with possible dementia is everyone’s business. Collateral history is of course essential, and provides much of the information regarding existing diagnoses and previous functioning. Without a collateral history it can be difficult to confidently identify those with a pre-existing diagnosis. Newham is one trust with a dementia registry. the collateral history is more useful than any diagnostic test eg AMTS, MMSE. Screening tests are not reliable in those who are not English speakers, and those with low levels of educational achievement.
The final message was to think about dementia, and to spend time getting a collateral history to facilitate diagnosis, but to leave formal diagnosis to the geriatricians.
Talking about Resuscitation: Dr Ashling Lillis
Dr Ashling Lillis had the unenviable task of providing a background to DNAR decision making, and translating the legalese of the recent UK High Court ruling R (David Tracey) vs 1) Cambridge University Hospitals 2) Secretary of State for Health. She did a fantastic job!

From: http://www.guardian.com
The Judicial Review describes CPR as: “a violent and invasive physical treatment used to attempt to maintain the circulation and breathing of a person whose heartbeat and/or breathing has stopped and to re-start the heart if possible. It involves repeated forceful compression of the bare chest to a depth of 5-6 centimetres at a compression rate of 100-120 per minute, attempted inflation of the lungs by forcing air or oxygen into the lungs often through a tube inserted into a patient’s windpipe, the injection of drugs into veins or into bones and the delivery of high-voltage electric shocks (defibrillation) across the bare chest.”
CPR was established in the 1960s for witnessed cardiac arrest from reversible causes. In the 1970s it became the standard treatment of all causes of cardiac arrest. The first DNACPR orders appeared in the 1970s. In-hospital outcomes have improved very little in the last 15 years.
- Peberdy, Mary Ann, et al. “Cardiopulmonary resuscitation of adults in the hospital: a report of 14 720 cardiac arrests from the National Registry of Cardiopulmonary Resuscitation.” Resuscitation 58.3 (2003): 297-308.
- Ebell, M. H. (1992). Prearrest predictors of survival following in-hospital cardiopulmonary resuscitation: a meta-analysis. The Journal of family practice, 34(5), 551-558.
Risk factors for non-survivalof CPR include co-morbidities, poor premorbid functional status, and age. Currently 80% of patients who die in hospital have a DNA-CPR order. They vary in format and wording, and there is a lack of standardisation. Newer forms include: treatment escalation plan; universal form of treatment options; and allow natural death form.
The case which prompted recent debate regarding DNA-CPR is R (David Tracey) vs 1) Cambridge University Hospitals 2) Secretary of State for Health, which you can read in full online. It provides details of the case of Janet Tracey, who was diagnosed with metastatic lung cancer (estimated prognosis 9 months). Just a few weeks later she was in a road traffic accident and had a cervical spine fracture. She was admitted to Neuro-critical care and was intubated. The ICU/anaesthetic team attempted to wean Mrs Tracey from the ventilator but this was unsuccessful. A DNA-CPR was completed. She was then successfully weaned from the ventilator. When Mrs Tracey’s daughter learned of the DNA-CPR she was horrified and the order was cancelled. Later Mrs Tracey’s condition deteriorated again. She said she did not wish to discuss resuscitation. Following a discussion withe her family, it was agreed that a second DNA-CPR order should be completed. She died two days later. The legal case focused on the first DNA-CPR order and whether this breached Mrs Tracey’s rights.
Article 8 of the Human Rights Act is the right to respect for private and family life. It was claimed that this right was breached:
- inadequate consultation
- lack of notification of the DNA-CPR decision
- no offer of a second opinion
- no DNA-CPR policy was made available
In this case there was failure to discuss the making of a DNA-CPR decision with a patient who had capacity and had expressed a clear wish to be involved in discussions about her care. Interestingly in a patient who is ‘at risk’ of cardiac arrest, failure to consider a decision about CPR may also be a breach of Article 8. An updated statement from the Resuscitation Council, Royal College of Nursing and BMA in 2014 responded to the ruling. It maintains the position that DNA-CPR decisions are medical decisions.
Following the ruling there is now a reinforced legal duty to discuss decisions about care with patients, particularly DNA-CPR decisions. This provides an opportunity to engage patients about informed decision making. In order to have meaningful conversations, it is important to be aware of the data related to DNA-CPR.
CPR outcomes in the elderly >70 were investigated in a meta-analysis of 11,337 patients by Gijn et al who found that survival to discharge varied with age: 18.7% of 70-79 year olds, 10.4% of 80-89 year olds, and 11.9% of 90+ year olds survive to discharge.
Successful CPR is associated with: rapid initiation of CPR; a VF/VT rhythm; and arrest in a critical care environment. Poor CPR success is associated with: metastatic malignancy; LV systolic dysfunction; severe sepsis; renal failure; poor functional status at baseline; a prognosis of <12 months from an established condition; and age >75 vs age <75 (trend for age). It is essential to also consider quality of life. The majority of CPR successes have a significant deterioration in functional status at a year (55-72%). Only 3-17% have a cerebral performance score of 1-2 (ie good neurological outcome).
In a Japanese study of 85,864 patients 42% had cerebral performance score 2+ at 6 months. In a UK study 774 patients 74% had a cerebral performance score of 2+ at 6 months. A score of 1-2 is sufficient cerebral function for ADLs. Chan et al looked at outcomes of 7000 elderly patients and found 63.7% survival in 65-74 year olds, 58.6% in 75-84 year olds, and 49.7% of >85 year olds.
Roch et al looked at 299 patients >80 years old admitted to ICU and found in-hospital mortality 55%, with 47% of survivors alive at 2 years, but with lower energy levels and lower functional status. Interestingly subjective quality of life scores were nit significantly different in ICU survivors and general population.
The QALY for CPR is £170,000. (NICE has a cut off of £25000 to approve treatments….)
If we all do lots of appropriate discussing and decision-making regarding DNA-CPR, we must communicate this to the community. Letters and phone calls to GPs help. Systems such as Co-ordinate My Care are great, if the right people have access.
Liver disease in pregnancy
Dr Aruna Dias armed us with some knowledge for the next time we get the dreaded call from the maternity wing. he covered three areas of liver disease in pregnancy: pregnancy specific liver diseases such as hyperemesis gravidarum, pre-eclampsi, HELLP and AFLP; coincident liver disease such as acute viral hepatitis, DILI, Budd-chiari and acute cholecystitis; and pre-existing liver disease such as chronic viral hepatitis, autoimmune hepatitis, and PBC. It turns out that abnormal LFTs in pregnancy are not uncommon:
LFTs should remain normal in pregnancy. However “normal-abnormalities” include a fall in albumin, urea and creatinine and rise in AFP throughout pregnancy, and a rise in ALP in the third trimester.
- Hyperemesis gravidarum has a prevalence of up to 2% in the first trimester, but should stop by 20 weeks. The liver is involved in 50% of cases. A rise in ALT is seen, with a smaller rise in bilirubin. Risk factors include high BMI, twins, diabetes, and hyperthyroidism. Treatment is with iv fluids, anti-emetics and vitamins.
- Intrahepatic cholestasis of pregnancy typically occurs in the 2nd and 3rd trimesters. Patients have pruritus without rash. Jaundice is rare (<10%). Bloods show a high ALT/AST and more moderate rise in bilirubin with a normal GGT. High bile acids increase the risk of stillbirth. Treatment is with ursodeoxycholic acid (alternative is rifampicin) and early delivery.
- Pre-eclampsia is the combination of hypertension (SBP >140mmHg DBP >90mmHg) and proteinuria. Risk factors include pre-existing hypertension, extremes of age, first pregnancy, and twin pregnancy. Eclampsia can lead to seizures and the death of the mother. Treatment is blood pressure control (labetalol, magnesium) and early delivery.
- HELLP (Haemolysis, Elevated Liver enzymes and Low Platelets) is a complication of severe pre-eclampsia. Haemolysis leads to high LDH and low haptoglobin. There is also high urinary bilirubin, low platelets, and high ALT.
- AFLP (Acute Fatty Liver of Pregnancy) is a severe but rare condition (1/10000) which occurs in the third trimester. It involves long chain fatty acid malabsorption and can co-exist with pre-eclampsia. It is difficult to diagnosis, and the Swansea criteria are used to facilitate diagnosis.
Nutrition
Dr Andrew Rochford grabbed our attention with some stark statistics on nutrition in the UK. Over 3 millions adults are malnourished, and it is twice as common in the elderly and those with chronic disease. 13-40% of inpatients are malnourished, with risk factors including being from a care home (52%) and being made nil by mouth >5 days.
- NICE Guideline CG32: Nutrition support in adults: Oral nutrition support, enteral tube feeding and parenteral nutrition (2006)
- NICE Quality Standard QS24: Quality standard for nutrition support in adults (2012)
Basic nutritional assessment should occur on admission to hospital and at a first clinic appointment. MUST is a screening tool which puts people into low, medium and high risk categories for malnutrition. It relies on BMI being properly calculated. Physical assessment is part of the nutritional assessment. Oedema may indicate protein depletion, poor mobility may be due to low muscle mass or neuropathy, and low mood may be due to apathy or depression. These can be caused by and contribute to malnutrition.
Contributors to poor nutrition include:
- poor intake – quality and quantity of food, appetite, investigations (NBM), medications (SE nausea)
- malabsorption – coeliac, cancer, oedema, abdo surgery
- increased losses – burns, fistulae, renal failure (protein loss)
Investigations include:
- bloods – haematinics, trace elements (selenium, vit A, zinc – not routine tests), B12, folate, iron, albumin (poor marker of nutrition as negative acute phase protein)
- stool – faecal elastase (pancreatic function), calprotectin (IBD)
We reflected on hospital food, and its’ lack of appeal. Although hospital meals will meet the nutritional requirements of a patient, it is often unappealing and not eaten, so this is meaningless. Family often bring in food, and this is to be encouraged. The CQC has a dignity and nutrition inspection programme which highlights areas of good and bad practice related to nutrition in hospitals and care homes.
Simple interventions can help. Using red trays to highlight patients who needed assistance at mealtimes decreased length of stay in rehab units. Many other interventions lack evidence. For example, protected mealtimes have poor evidence for increasing nutritional intake, but are associated with fewer complaints and increased satisfaction with food.
Assessing nutritional support needs requires an understanding of variations in basal metabolic rate and changes in energy expenditure as well as nutritional intake. A number of equations are available to facilitate calculation of basal metabolic rate, which will be familiar to dieticians. These include the Henry and Schofield equations. Overfeeding should be avoided as it leads to diarrhoea and increased physiological stress. Adult nutritional requirements are: 25-35kcal/kg, 0.8-1.5g protein/kg, 1mmol Na/kg, 1mmol K/kg, electrolytes (magnesium, phosphate etc), micronutrients and 30-35ml fluid/kg. NB 1 sando-K tablet = 12mmol K.
Oral supplements come in different strengths: 1, 1.5 or 2kcal/ml. They should be given at 10, 14 and 20 (not mealtimes, to encourage normal eating). They are cost effective as they decrease length of stay. Patients can be safely fed via NG tube for 6 weeks. Be careful re: NG tube placement. Misplacement is a never event. If you are unsure of how to assess NG placement do an online training module from Salford Hospital and download the Southamptom app.
PEG tubes are a more longterm solution. You may be called overnight if a PEG tube falls out. If it has been in 6/52 or more a tract will have been established. You should immediately place a foley catheter in the hole to maintain the tract. The PEG can be replaced by the specialist team the next day. If you do nothing the tract will close within 2 hours.
Parenteral nutrition should only be used if other alternatives are not possible, since it is not safe. There are mechanical, infective and metabolic risks. If the patient has a fever >38 you should stop parenteral nutrition for 48 hours. An NCEPOD report found that 81% of parenteral nutrition was poorly prescribed, 29% was clinically inappropriate, and 49% of complications were avoidable (poor care and documentation of central venous catheter).
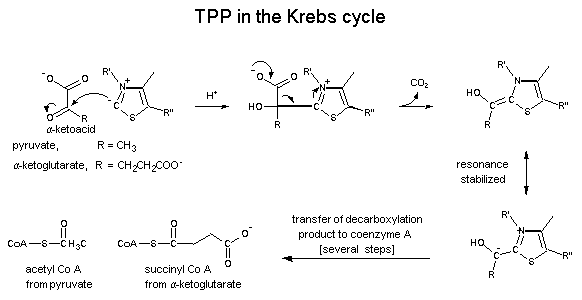
Re-feeding syndrome is a potential problem following establishment of any form of feeding. Thiamine pyrophasphate (TPP) is needed for pyruvate acid –>acetyl CoA, which is needed for the Krebs cycle.
A study of the biochemical and endocrine abnormalities of re-feeding syndrome was undertaken using a volunteer(!) who fasted for 44 days. Lack of calorie intake with free access to water resulted in 25% loss of body weight. During early re-feeding, marked hypophosphataemia, haemodilution and slight oedema developed. Vitamins B1, B12 and B6 were depleted while serum free fatty acids, ketone bodies and zinc levels were abnormally high; abnormal liver function developed over the first week. The recommendations were that careful attention should be paid to electrolytes during re-feeding. If K <3.0 the patient should be in a HDU for more invasive monitoring and faster electrolyte replacement.
Feeding often brings in ethical issues, particularly in those who may be nearing the end of life. Both the RCP and BSG produce guidelines on this subject.




Discussion
No comments yet.